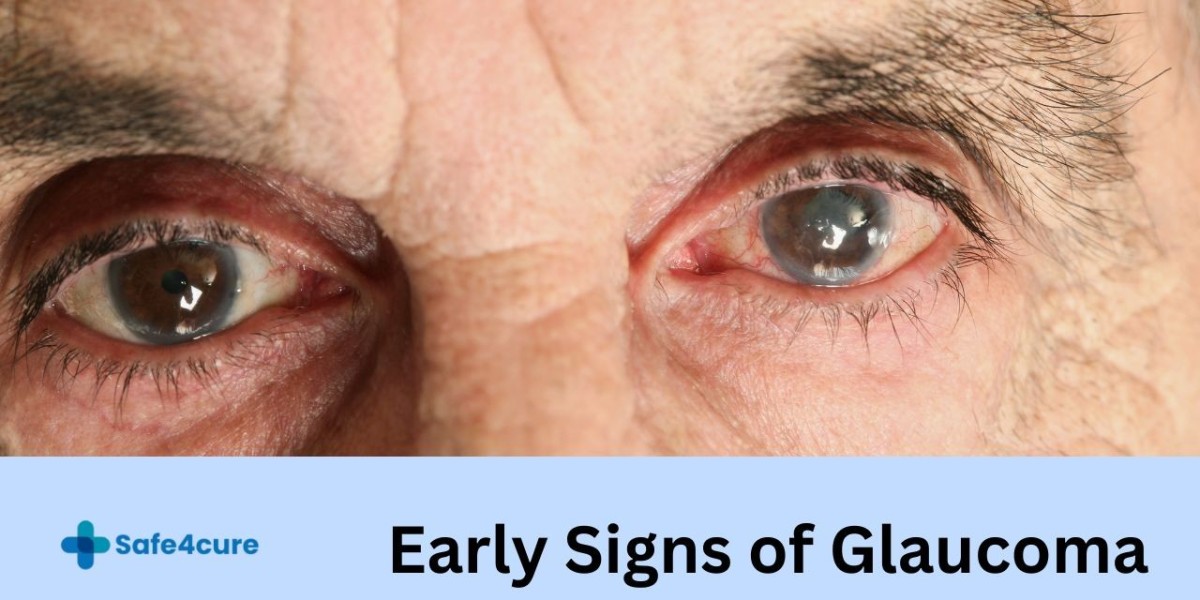
We are living in a screen-dominated world. From smartphones and laptops to tablets and TVs, Americans now spend more than seven hours each day looking at digital screens. While this digital revolution has transformed how we work, learn, and communicate, it has also raised important concerns about eye health—especially for individuals managing glaucoma. Glaucoma is a chronic eye condition in which elevated intraocular pressure (IOP) gradually damages the optic nerve, potentially leading to irreversible vision loss. If you have been diagnosed with glaucoma or are experiencing increased eye pressure, you may wonder whether prolonged screen time is making the condition worse.
The encouraging news is that early detection and proper treatment with medications such as Lumigan and Lumigan 0.03 can help safeguard your vision. Lumigan 0.1 is also used to treat glaucoma and may contribute to the loss of eyelashes in some individuals. Understanding how digital screen exposure interacts with glaucoma-related eye pressure is essential for anyone trying to protect their eye health in today’s technology-driven environment.
Understanding Glaucoma and Eye Pressure
What Is Glaucoma?
Glaucoma definition: it's a group of eye diseases that damage the optic nerve, which connects your eye to your brain. This damage typically occurs when fluid builds up in the front part of your eye, increasing pressure and gradually harming the nerve fibers.
The glaucoma meaning goes beyond just high eye pressure, though. It represents a serious threat to vision that often progresses silently. There are several types:
Open angle glaucoma is the most common form in the United States, developing slowly as drainage canals become clogged over time. Angle-closure glaucoma happens when the iris blocks drainage angles suddenly or gradually. Normal-tension glaucoma damages the optic nerve even with normal pressure levels. Secondary glaucoma results from other eye conditions, injuries, or medications.
What Causes Increased Eye Pressure?
Understanding the causes of glaucoma begins with knowing how the eye naturally maintains intraocular pressure (IOP). The eye continuously produces a clear, nourishing fluid known as aqueous humor. Under normal conditions, this fluid drains out through microscopic channels that help regulate pressure. When these drainage pathways become blocked or the eye produces excess fluid, IOP begins to rise.
A healthy eye pressure level typically ranges from 12–22 mmHg. Once the pressure consistently climbs above this range, the risk of developing glaucoma increases significantly. Several factors drive this elevation, including advancing age (especially after 60), genetic predisposition, medical conditions such as hypertension or diabetes, the use of certain medications, and lifestyle triggers like prolonged near-focus tasks—particularly long hours spent on digital screens.
For individuals already experiencing high eye pressure or early glaucoma symptoms, medications such as Lumigan 0.03 are often prescribed. Lumigan 0.03 helps reduce IOP by improving fluid drainage from the eye and is typically used once at night, which fits well even for those dealing with sleep-related disruptions or irregular routines. Many patients also appreciate its convenient dosing schedule, long-lasting pressure-lowering effect, and suitability for chronic glaucoma management when used as directed.
Digital Screen Exposure and Its Connection to Eye Pressure
How Screen Time Affects the Eyes
When you're absorbed in your screen, several changes occur in your eyes. Your blink rate drops dramatically—from about 15-20 blinks per minute to just 5-7 blinks. This leads to dry, irritated eyes. Your eye muscles work overtime to maintain focus at close range, causing accommodation stress. Some research suggests prolonged near-focus tasks may temporarily alter ocular blood flow.
Can Screen Time Increase Intraocular Pressure (IOP)?
Here's what research tells us: while screen time doesn't directly cause glaucoma, studies indicate that prolonged near-focus activities may cause temporary spikes in IOP. For someone with healthy eyes, these small fluctuations usually aren't concerning. However, for glaucoma patients, even temporary increases can be problematic.
Several factors influence how screens affect what is glaucoma of the eye pressure:
Posture matters. Looking down at your phone or tablet can increase pressure compared to viewing at eye level. Screen distance plays a role—closer screens require more eye muscle effort. Blue light exposure from screens has been studied, though its direct impact on IOP remains debated. Usage patterns make a difference; continuous 8-hour sessions affect eyes differently than broken-up screen time with regular breaks.
Symptoms to Watch If You Have Glaucoma
If you have glaucoma eyes and spend significant time on screens, monitor these glaucoma symptoms:
- Eye pain or discomfort that worsens after screen use
- Headaches, particularly around the temples or behind the eyes
- Blurred vision that takes time to refocus
- Seeing halos around lights, especially at night
- Increased sensitivity when using digital devices
These warning signs shouldn't be ignored, as they may indicate your glaucoma treatment plan needs adjustment.
Managing Glaucoma in a Digital World
Lifestyle Adjustments to Reduce Screen-Related Eye Pressure
You don't have to abandon technology to protect your eyes. Smart habits can make a huge difference:
Follow the 20-20-20 rule: Every 20 minutes, look at something 20 feet away for at least 20 seconds. This simple practice gives your eye muscles a break.
Optimize your screen settings. Reduce brightness to match your surroundings, increase text size to reduce strain, and adjust contrast for comfortable viewing.
Mind your posture and distance. Position screens at arm's length and slightly below eye level. Avoid lying down while using devices.
Limit continuous sessions. Take a 10-15 minute break every hour during work or gaming.
Use protective measures. Anti-glare screen filters and blue light blocking glasses may provide additional comfort, though evidence on IOP reduction is limited.
Importance of Regular Eye Check-ups
If your job involves extensive computer work or you're a heavy screen user, regular IOP monitoring becomes even more critical. Your eye specialist can track changes in your optic nerve health over time and detect problems early—when treatment is most effective. For high-risk individuals, more frequent screenings may be recommended.
Role of Medications in Controlling Eye Pressure
Overview of Lumigan (Bimatoprost)
Lumigan is a prostaglandin analog medication that effectively lowers elevated eye pressure in glaucoma patients. It's often prescribed as a first-line treatment or combined with other therapies for better pressure control.
What Is Lumigan 0.03?
Lumigan 0.03 refers to a specific formulation containing 0.03% bimatoprost. This concentration has been shown to effectively reduce IOP while minimizing side effects. Some patients may also encounter references to Lumigan 0.1 or Lumigan 0.3 (which is 0.3 mg/mL, equivalent to 0.03%), but your doctor will determine the right strength for your situation.
The medication is typically applied once daily in the evening, making it convenient for busy professionals and screen users who need reliable glaucoma treatment without frequent dosing.
How Lumigan Works
Lumigan works by increasing uveoscleral outflow—essentially helping fluid drain more efficiently from your eye. This mechanism helps maintain stable eye pressure throughout the day, which is particularly valuable if you have long hours of screen exposure.
By consistently controlling IOP, Lumigan reduces the risk of optic nerve damage and progressive vision loss—the ultimate goal in glaucoma management.
Potential Side Effects
Most people tolerate Lumigan well, but be aware of possible effects:
- Temporary eye redness (usually mild)
- Increased eyelash growth and thickness
- Mild stinging or irritation upon application
- Gradual darkening of the iris or eyelid skin (permanent changes)
Always discuss any concerns with your ophthalmologist.
Additional Tips for Reducing Eye Strain with Glaucoma
Beyond medication and screen breaks, these strategies support overall eye health:
Use lubricating eye drops to combat screen-induced dryness. Avoid marathon reading sessions on phones or tablets—opt for audiobooks when possible. Ensure proper lighting—avoid screen use in complete darkness and eliminate glare from windows. Schedule screen-free hours, especially before bedtime to improve sleep quality. Stay physically active, as moderate exercise can help reduce eye pressure naturally.
Does Blue Light Worsen Glaucoma?
Blue light has become a hot topic in eye health discussions. Digital screens emit significant blue light, which penetrates deeper into the eye than other wavelengths. Some studies suggest excessive blue light exposure may affect retinal cells over time.
However, current scientific evidence doesn't conclusively link blue light directly to increased IOP or accelerated glaucoma progression. The concern is more about potential long-term retinal damage and sleep disruption rather than immediate pressure spikes.
That said, blue light filters and glasses won't hurt and may improve comfort during extended screen sessions.
Diet and Supplements for Better Eye Health
Your nutrition plays a supporting role in glaucoma management:
Omega-3 fatty acids found in fish, flaxseeds, and walnuts support overall eye health. Antioxidants including vitamins A, C, and E help protect against oxidative stress. Dark leafy greens, carrots, citrus fruits, and nuts are excellent sources.
Stay hydrated but be mindful of drinking large amounts of fluid quickly, which can temporarily increase eye pressure. Limit caffeine, as high intake may cause short-term IOP spikes in some people.
While supplements can't replace glaucoma treatment like Lumigan, they contribute to comprehensive eye care.
When to Consult an Eye Specialist
Contact your ophthalmologist immediately if you experience:
- Sudden, severe eye pain
- Rapid vision changes or loss
- Persistent headaches that don't respond to usual remedies
- Symptoms that worsen despite using Lumigan as prescribed
- Any new visual disturbances like halos or blind spots
Early intervention can prevent irreversible damage.
Frequently Asked Questions (FAQs)
1. Can screen time directly cause glaucoma?
No, screen time does not cause glaucoma. Glaucoma develops due to genetic factors, age, and other medical conditions. However, excessive screen use can exacerbate symptoms or discomfort in those already diagnosed with the condition.
2. Does screen time increase eye pressure?
Research suggests that prolonged near-focus activities, including extended screen use, may temporarily elevate IOP in some individuals. This effect appears more pronounced in people with existing glaucoma, making pressure management even more important.
3. Is Lumigan effective for screen-induced eye strain?
Lumigan specifically targets elevated eye pressure, not eye strain symptoms. While it won't relieve screen fatigue directly, it protects your optic nerve by maintaining healthy pressure levels—critical for frequent screen users with glaucoma.
4. What is the difference between Lumigan and Lumigan 0.03?
Lumigan 0.03 indicates the specific concentration (0.03% bimatoprost). Various formulations exist, but your ophthalmologist will prescribe the appropriate strength based on your individual needs and response to treatment.
5. How long does Lumigan take to work?
Most patients notice IOP reduction within 3-4 weeks of consistent daily use. Maximum benefit typically occurs after 8-12 weeks. Regular monitoring ensures the medication is working effectively.